Back in the 1990s Veech's lab noted that supra maximal insulin, combined with glucose at 11mmol/l, markedly improved the ability of an isolated rat heart to pump oxygenated perfusion fluid compared with glucose alone. The mechanism of the effect was not explicable from their model but was very clear cut and the time scale of onset suggested a covalent bonding process.
Substrate signaling by insulin: a ketone bodies ratio mimics insulin action in heart
Substrate signaling by insulin: a ketone bodies ratio mimics insulin action in heart
Macroscopically, the amount of work done per mole of oxygen consumed increased. As this was without an increase in glycolysis the implication is that insulin increases the coupling of mitochondria.
I was left with the idea at the time, reinforced occasionally by other finds, that insulin was has a major effect of increasing coupling within mitochondria.
I was left with the idea at the time, reinforced occasionally by other finds, that insulin was has a major effect of increasing coupling within mitochondria.
Insulin clearly has many, many effects within a cell. It's not possible to examine any of these using isolated mitochondrial preparations because they have no cytoplasm to respond to insulin. You need intact cells.
I recently came across this rather nice paper:
It looks at an assortment of muscle derived cells in much the same way as mitochondrial preparations examine mitochondrial performance, but here whole cells used, a small step closer to reality than isolated mitochondria. They have intact cytoplasm so can function on "normal" substrates such as glucose or palmitic acid. The cells are not even "permeabilised".
They used standard mitochondrial techniques such as full uncoupling with FCCP to assess the maximum possible oxygen consumption and oligomycin to assess peak oxygen consumption from proton leak in the absence of a functional ATP synthase. So they can provide standard mitochondrial study parameters like respiratory control ratio and make estimates of the degree of (un)coupling of respiration and of the efficiency of ATP generation.
All good but even better they then went on to look at the effect of fairly physiological concentrations of insulin on these parameters. And to look at the effect of palmitate alone and palmitate in combination with insulin.
They are looking at mitochondrial function within intact cells, with functional cell surface receptors and cytoplasmic signalling cascades. Insulin was used at 10nmol/l (10,000pmol/l) which is only just above peak post prandial levels and even their 100nmol/l dose is still way below the millimolar concentrations commonly used to assess the effects of supra maximal insulin stimulation on cell preparations.
Their palmitate dose rate is hard to assess as they presented it bound to albumin with an estimated free palmitate of 20nmol/l, ie 0.02micromol/l. Almost every other study simply measures/specifies total palmitate in solution so making comparisons is hard. Obviously the 400-2000micromol/l of FFAs which are normal in fasted human plasma are almost completely albumin bound, so it's hard to tell if the estimated 20nmol/l of free palmitate used in the study is high or low. It certainly has an effect.
These are the graphs of oxygen consumption from the human derived muscle cells/myotubes:
The graphs are not intuitive. First, everything is normalised to the rate of oxygen consumption under the influence of oligomycin (between times 20 and 40 minutes) ie state 4oligomycin, and are expressed as a percentage of this. So the sections of the graph in the "dip" after the line labelled "OLI" are baseline and labelled 100, ie 100%.
Under oligomycin there is a complete blockade of ATP synthase so any oxygen consumption has to be facilitated by uncoupling. The absolute values will not be identical with vs without insulin, they are just deliberately aligned at 100. The absolute values will differ based on the activity of uncoupling proteins.
Once FCCP is added there is complete uncoupling of all respiration (while ATP synthase still remains blocked with oligomycin) and so this represents the maximum possible flow of electrons down the ETC to complex IV, with no buildup of proton gradient to inhibit this. These peak values are probably identical whether insulin has or hadn't been applied because FCCP is supra maximal in its uncoupling so subtleties of UCPs become irrelevant. No one has added palmitoylcarnitine either.
This shows as a greater percentage *increase* when insulin has been applied earlier, ie the oligomycin phase had different absolute oxygen consumptions with or without insulin. I think it's just convention to set up the graphs as they are.
So glucose + insulin couples respiration compared to glucose without insulin.
Which reiterates Veech's findings.
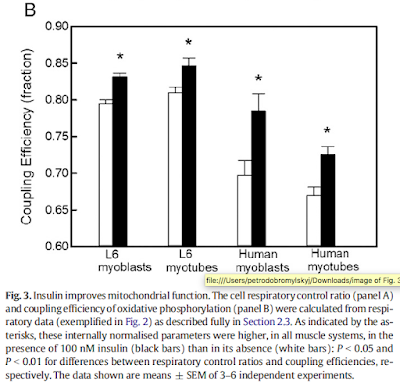
Okay. So we can calculate the coupling efficiency of mitochondria respiring on glucose with or w/o insulin and express it as a fraction of unity. Insulin always increases the coupling of respiration when oxidising glucose. Black bars with insulin:
The study didn't look at delta psi or ROS generation so we have no way of knowing exactly what happens to these parameters.
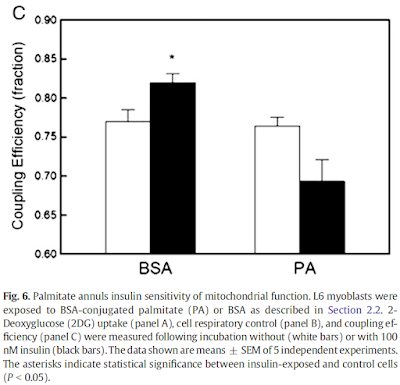
Adding palmitate completely blocks (and probably (ns) decreases) the increase in respiratory coupling seen when insulin is added to glucose. Right hand columns labelled as added PA:
The change downward looks to have come very close to statistical significance. This suggest that small (possibly) doses of palmitate negate insulin's coupling effect and trend towards actively reversing it.
What is also interesting is the left hand pair of bars. The white bar is insulin + glucose and the black bar is insulin, glucose and "empty" bovine serum albumin (BSA). The BSA produces a statistically significant increase in coupling of respiration. This is in a cell prep which has not been treated with exogenous fatty acids. There are enough fatty acids "floating around" to interfere with insulin's coupling action on mitochondria.
My assumption is that the empty BSA scavenges free fatty acids by supplying a sequestration site for any FFAs in the culture. Reminiscent of the effect of carnitine in a previous post.
Let's make this completely clear: Mitochondria in cells exposed to insulin are more coupled compared to those without insulin. Adding extra palmitic acid reduces this extra coupling. Removing background levels of free fatty acids enhances insulin's coupling effect.
Insulin is an enhancer of coupling in the mitochondria of intact cells. It's effect appears to be mediated through changes in free fatty acid availability which are known mediators of activation of uncoupling proteins.
TLDR: All isolated mitochondrial preparations are devoid of insulin signalling so will automatically be uncoupled to some degree, which goes some way to explaining continued oxygen consumption under oligomycin. Especially using supra maximal NADH generating substrates. But it doesn't help explain the regulation of membrane potential to around 180mV under high substrate supply.
Other things might.
Peter


18 comments:
Totally off topic, but recently ive heard that when you fast an overweight cat it will develop fatty liver, while this is not a problem in humans (rather the opposite).
So i wonder, why does this occur in cats? Whats the differnence in cat physiology?
And secondly: whats a healthy way for a cat to lose weight?
I'm going to guess that a raw meat diet is the best way to make a cat lose weight. I had a cat who got fat and lost all his teeth on a diet of kibble. I'm ashamed it took me so long to realize that what was good for me was probably even better for my cats, carbwise. My current cat gets raw meat and hunts a lot, no dry food at all. She just turned 10 and is svelte and active.
The full blown syndrome is hepatic lipidosis and carries a high fatality rate. My guess is that it is secondary to overwhelming adipocyte fat loss from high basal lipolysis which isn't being exported from hepatocytes fast enough. Oddly enough a fish oil supplement is highly protective against fatty liver during "planned" weight loss. Sone ideas as to why are in Sauer's work in https://high-fat-nutrition.blogspot.com/2013/09/omega-3s-and-g-protein-coupled-receptors.html for some idea.
My cats keep kicking my ideas of obesity control down the road!
Peter
cavenewt,
Don't know when and where I read it, but my understanding is cats are obligate carnivores, so I suppose feeding them vegetable matter is not recommended.
The other day on Twitter I saw a video of a cow (or bull) nuzzling a kitten. Thought I'd bookmarked it, but I can't find it. The comments were full of, "Oh, how sweet" and "We have so much to learn from animals".
But there was also a video of a cow eating a young chick and another of a horse doing the same.
https://twitter.com/vidfindr/status/1284618429266161664
Kind of made me wonder if the "nuzzling" cow was just trying to decide whether to eat the kitten. Apparently herbivores like the occasional protein supplement.
LA_Bob. I have always known that cats are "obligate carnivores" but wasn't sure exactly what that meant. It's tempting to think that this means they can only eat meat and nothing else. So I looked it up. That's not quite right; obligate carnivores have to eat a certain amount of meat because they can't create some vital nutrients from plants, fungi, or bacteria. This is from encyclopedia Britannica: "In particular, obligate carnivores lack the enzyme needed to split carotene, obtained from plants, into vitamin A. Instead, these animals obtain vitamin A from the liver of their prey. Obligate carnivores are similarly unable to synthesize some essential very-long-chain, highly unsaturated fatty acids that other animals can make from shorter fatty acids found in plants." Dogs are more omnivorous than cats, and supposedly can do better with more vegetable matter.
I read a book a few years ago titled Dogs, Dog Food, and Dogma. It's like Good Calories, Bad Calories for pets, specially since the author makes numerous references to Gary Taubes. I highly recommend it for anyone who has dogs or cats – it's not just about dogs. In addition to the nutritional aspects, he goes into great detail about how the veterinary and pet food industries are every bit as culpable in the ill health of pets as Big Food and Big Pharma are in humans.
Mike Eades likes to post vintage films of things like people standing in line for the first Star Wars movie, and pointing out how slim everyone is. Unlike today, where so many people are, to use an adjective from Brave New World, pneumatic. I'm old enough to remember that time. Not only people were slim, but nobody's pet was fat or cancerous. It's upsetting to see funny Internet cat videos of poor bloated roly-poly cats. I'm sure crappy dry pet food has a lot to answer for.
One rather appalling sidenote…in looking up a definition for obligate carnivore, I ran across a book by that exact title on Amazon. It's all about how to impose a vegan diet on your pets. And how it's good for them. Words fail me.
cavenewt, thanks for the correction. I did indeed conflate "obligate carnivore" with "exclusively carnivorous".
I have also seen claims vegan diets are just wonderful for cats and dogs. Yeah, horrifying.
OT: Lp(a)
Not that much of interest in this paper - but learned one thing - the evolution from plasminogen.
This greatly supports Kendick's narrative that CAD is a thrombotic disease - not a disease of lipids.
https://www.atherosclerosis-journal.com/article/S0021-9150(22)00180-0/fulltext
This is even more off topic but too tasty to not share --- fresh veg are very expensive in Aus atm due to widespread floods in veg growing areas. The price of snow peas just hit $42 / kilo, more than most cuts of beef. Hmm, peas or rump steak for dinner? Veganism has become the expensive option.
'Social media users were shocked by the inflated price.
“Sooner or later, Lobster will be cheaper than salad!” said one.'
Too late.
'“Sooner or later, Lobster will be cheaper than salad!” said one.'
'Tis a consummation devoutly to be wished!
Just an idea, insulin clean up FFA by making triglycerides, isn't it protecive mechanism? FFA are intended to modulate fat metabolism by GPx, not to modulate glucose metabolism. If this happens, cell will overload with fuel.
@mct4health
Quite possible that one of the roles is to protect use from other bad-things. Not sure if that still works if the liver is insulin resistant?
But, elevated insulin is correlated with many bad things health-wise. High Trygly is also correlated with things like CAD.
Insulin does a LOT of things:
Insulin also has MANY other effects (assuming that the tissue in question is not resistant):
controlling storage of fat - Decreased lipolysis
as a growth factor.
glycogen synthesis
Increased cellular potassium uptake
decreases production of glucose from noncarbohydrate substrates
Increased lipid synthesis
Increased production of trygly from fatty acids
decreased breakdown of proteins
Decreased autophagy - decreased level of degradation of damaged organelles. Postprandial levels inhibit autophagy completely.
forces cells to absorb circulating amino acids
forces arterial wall muscle to relax
Increase in the secretion of hydrochloric acid in the stomach
Decreased renal sodium excretion
enhances learning and memory
increased fertility
In the bigger picture -
- Liver becomes insulin resistant first, muscles second, adipocytes last.
- Insulin levels in the obese remain about 10 times those of a normal person even under complete starvation.
Something to consider - these numbers:
https://news.gallup.com/poll/7264/personal-weight-situation.aspx
In my mind, it is clear that the T2D pandemic is a magnitude bigger health issue than the virus - and we are not dealing with it.
-- Which reminds me - don't like twitter - but this is telling:
https://twitter.com/IFandKETOxx/status/1539594213792309249
https://twitter.com/DrEades/status/1539357417808482304?cxt=HHwWgMCy7cza8twqAAAA
My playground in the 1960's didn't really look different. When I go out in public, I see flaccid people (low muscle mass), something about the skin texture is off - even in the young - my hunch is this is effecting sex hormones as well (dropping birth rate) - brain function? Seems like an actual health crises to me.
Something about the modernity - most likely diet has caused this pandemic of T2D. Seed oils are at the top of my list.
Other possibilities are the additives - do preservatives change bowel flora enough to cause changes? Endocrine disruptors in plastics? Addictive flavor enhancers? Big correlation with ultra-processed-foods(what I call food-like-substances).
@karl
I completely agree. Just one little point, glucose stimulated insulin secretion is modulated by FFA when fasting. In this paper they completely erased insulin secretion by stopping lipolysis. Different free FA has different effect. I see FFA as key to understand it and it is not researched enough.
https://diabetes.diabetesjournals.org/content/diabetes/51/1/7.full.pdf
@mct4health
I agree - it begs the question why? Is this targeted at the liver or adipose tissue? How did that evolve? If insulin goes down - lipolysis goes up producing more FFA? Less production of trygly. But lipid synthesis would also go down. I'm having trouble making sense of it - perhaps Petro can walk us through a possible narrative?
Early work in CAD health was focused on Trygly levels - but I think it might have been a proxy for FFA. High FFA is not normal - could be we are looking at situations that we did not evolve for? FFA are independently associated with higher all-cause-mortality - but - FFA is not a single thing - we need data on the different types of FFA.
Also, an important thing to remember - FFA is not 'a thing' It is 'many things'. If someone has been eating half their calories as LA for years - during fasting, their FFA is going to different than someone that has been eating a 1950's diet. Obvious experiments come to mind.
,.,.
What is maddening, is it seems there is no end of money they can print - but there is no serious program to get to the bottom of the huge T2D pandemic that is killing people - ruining their lives etc.. Instead the money goes to Pharma - or guarding old narratives - they are very careful that nothing gets funded that has a chance of embarrassing the old guard or threaten Pharma profits.
I suspect that there is one - or a few things that account for the majority of T2D - as we sit by and see so many sick - and dying of a preventable disease. This was already an obvious problem in the '90's - decades have passed.
@karl
I suspect that main problem could be that some FFA (like LA) modulate sensitivity of cells to hypoxia. Like in the well known rat heart study where LA caused cell death. Cells cannot properly prepare, so the normal situation can lead to necrosis, inflammation, autoimmune reactions, pain, loss of tissue etc. And all that can be explained by excessive activity of glutathion peroxidase caused by free LA. But nobody suspect LA, that "super healthy" fat that lowers cholesterol. And nobody knows about its influence on GPx, H2O2 signalling and HIF1A stabilisation.
Here's a lovely bit of rancid lipid research from the late 80's. I love the earnestness of their enquiry --- food manufacturing for profit obviously calls for the investigation of every possible optimisation method. It's more trustworthy than medical research but not less awful.
"Influence of oxidised dietary oil and antioxidant supplementation on membrane-bound lipid stability in broiler meat"
https://pubmed.ncbi.nlm.nih.gov/2627662/
" Oxidised oil in the broiler diets induced rapid oxidation of the menbrane‐bound (sic) lipids"
Sorry for posting off topic, but coudn't resist sharing this gem:
https://www.theguardian.com/society/2022/jul/11/adding-salt-table-food-linked-earlier-death-study
Last I remember from a presentation by Malcolm Kendrick based on a Scottish heart study, those with the highest sodium consumption lived longest and had the least heart trouble. I think it has also long been established that excess sodium leads to higher blood pressure only in about 1-2% of the population who have a particular gene defect.
There may be a grain of thruth in that those who regularly consume ready-made TV-dinners and crisps are used to the taste of salt and hence will season real food at the table. Those dinners and crisps are usually made with copious amounts of heart healthy seed oils, so there you go.
On myself, I have observed that after stocking up in a French supermarket with plenty of delicious salted butter and cheese and living off that stockpile, I get into salt fatigue, i.e. I get a permanently salty feeling and tend to avoid extra salt but my BP stays perfectly normal.
@Eric
This is a good example of how a correlation is not helpful - My hunch is a little is good - too much is bad. I think Kendrick probably has this correct - but once again, my hunch is not the same as 'knowing'. Note how the guardian journalists completely failed at understanding what science means.
Could be that the people that use salt - overeat more than others - not related to the salt - but the taste.
The people I know that eat salty stuff - tend to eat a HUGE amount of salt - most restaurants seem to think more salt is better - too much does not taste good to me. Am I strange?
To really understand salt - I think one would have to control for potassium, magnesium, zinc.. what I see in the literature is just quick and dirty correlations that are mostly worthless.
The amount can change one's sense of taste - after eating low carb for decades now - I find most sweets overpowering - unpalatable - I used to like sweet treats..
To follow Eric off-piste…
My understanding about salt and blood pressure it is that it was simply an assumption based on osmosis, with no real evidence. No doubt this was a bolstered by sketchy epidemiological studies like the one in The Guardian that Eric linked.
Most people here are probably familiar with Gary Taubes' is 2012 article in the New York Times, "Salt, We Misjudged You", which says 'With nearly everyone focused on the supposed benefits of salt restriction, little research was done to look at the potential dangers. But four years ago, Italian researchers began publishing the results from a series of clinical trials, all of which reported that, among patients with heart failure, reducing salt consumption increased the risk of death...Those trials have been followed by a slew of studies suggesting that reducing sodium to anything like what government policy refers to as a “safe upper limit” is likely to do more harm than good. These covered some 100,000 people in more than 30 countries...'
http://www.nytimes.com/2012/06/03/opinion/sunday/we-only-think-we-know-the-truth-about-salt.html
He also had a 1998 article on the controversy around salt research which is not paywalled: "The Political Science of Salt" http://garytaubes.com/wp-content/uploads/2011/08/science-political-science-of-salt1.pdf
Both articles describe the minimalizing of research going against the mainstream narrative in ways that are very similar to what we see today with Covid.
Post a Comment